Non-Surgical Treatment That’s Replacing Surgery in 2025: Embolisation Explained''
For decades, surgery was the default option for treating many conditions — from tumors to fibroids to abnormal blood vessels. But it’s 2026, we are evolving along with this artificial intelligence.
One minimally invasive procedure is quietly reshaping modern medicine: embolisation.
Used across specialties like vascular medicine, embolisation is now replacing traditional surgery in thousands of cases each year — with less pain, fewer risks, and much faster recovery.
So what exactly is embolisation, and why is it becoming such a big deal?
What Is Embolisation?

Embolisation is a non-surgical medical procedure that treats disease by blocking blood flow to a specific area of the body.
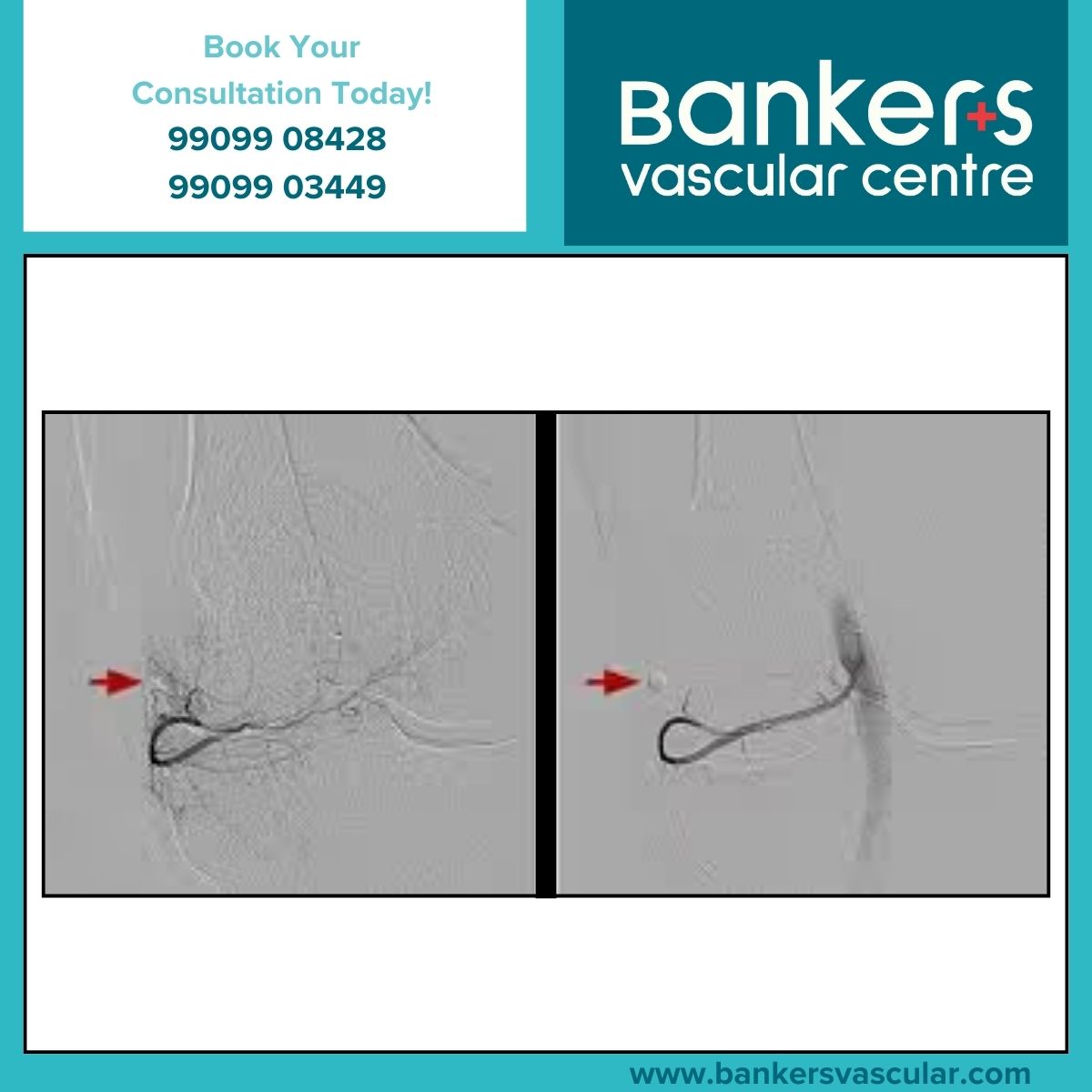
Instead of making large incisions, doctors insert a tiny catheter through a small puncture in the skin — usually in the wrist or groin. Using real-time imaging, the catheter is guided through the blood vessels directly to the problem area.
Once in place, embolisation materials (such as microscopic particles, coils, or medical glue) are released to block the targeted blood supply. Without blood flow, abnormal tissue shrinks, bleeding stops, or symptoms improve.
No stitches. No large scars. Often no general anesthesia.
Why Embolisation Is Replacing Surgery in 2025
1. It’s Minimally Invasive
Traditional surgery requires cutting through skin and tissue. Embolisation uses only a needle-sized entry point, dramatically reducing trauma to the body.
2. Faster Recovery
Most patients return to normal activities within days, not weeks. Many embolisation procedures are done as same-day outpatient treatments.
3. Lower Risk of Complications
Because there are no large incisions, risks like infection, excessive bleeding, and long hospital stays are significantly reduced.
4. Precision Treatment
Embolisation targets only the affected blood vessels, leaving surrounding healthy tissue largely untouched.
Conditions Where Embolisation Is Replacing Surgery
Chronic Pain Conditions
One of the fastest-growing uses of embolisation in 2025 is chronic musculoskeletal pain, especially when surgery has failed or isn’t ideal.
This approach is often called pain embolisation.
Knee Pain (Osteoarthritis)
In patients with chronic knee pain, abnormal inflammatory blood vessels can develop around the joint. Genicular artery embolisation reduces this excess blood flow, helping relieve pain and improve mobility — without knee replacement surgery.
Frozen Shoulder (Adhesive Capsulitis)
Frozen shoulder is associated with chronic inflammation and abnormal vascular growth. Embolisation can reduce this inflammation, leading to improved range of motion and pain relief, often avoiding invasive shoulder surgery.

Heel Pain (Plantar Fasciitis & Achilles Tendinopathy)
Chronic heel pain can be driven by persistent inflammation and abnormal microvessels. Embolisation targets these vessels, offering relief when physical therapy and injections have failed — without surgical release.
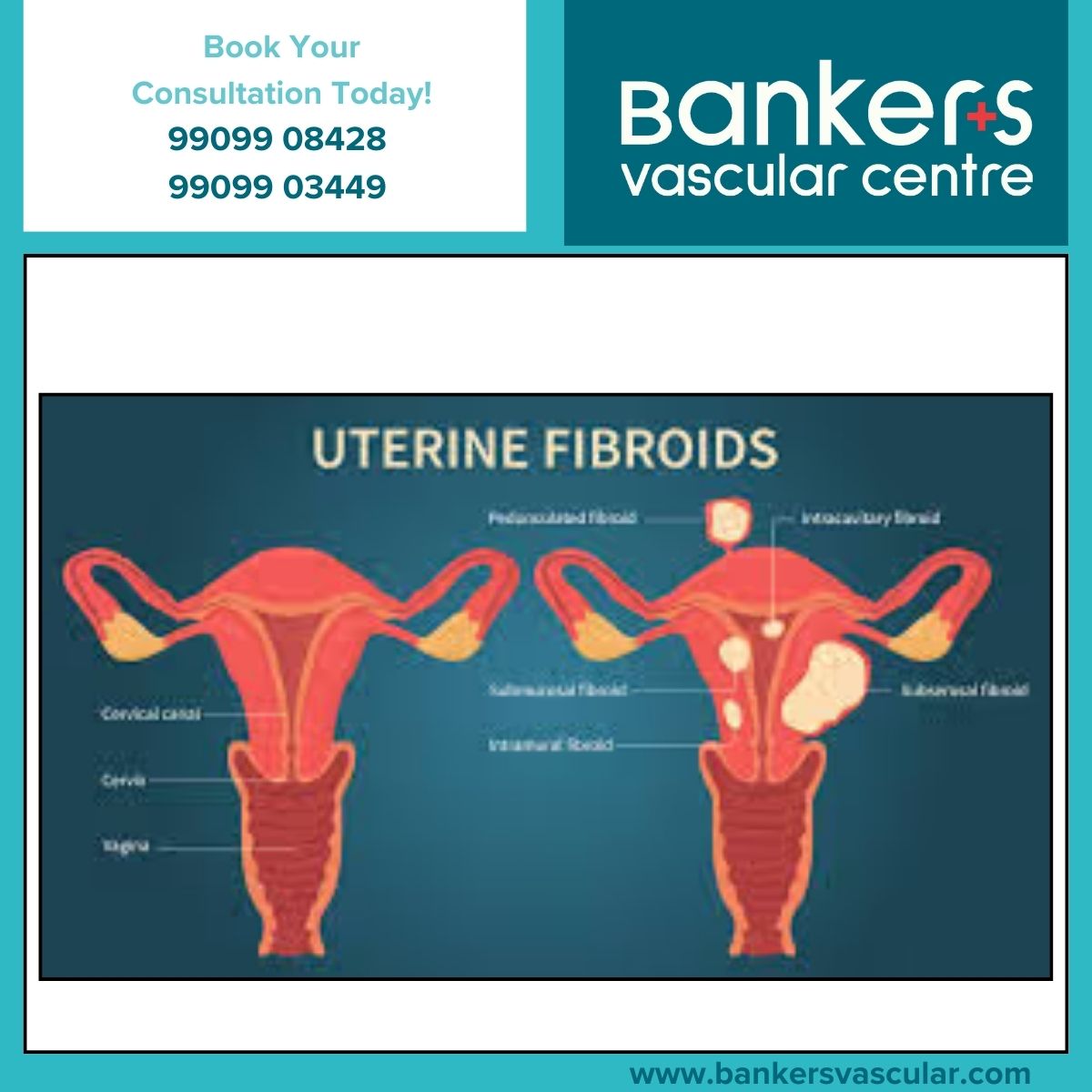
Uterine Fibroids
Uterine Fibroid Embolisation (UFE) is now a widely used alternative to hysterectomy or myomectomy. By cutting off blood flow to fibroids, they shrink naturally, reducing heavy bleeding and pain — without removing the uterus.
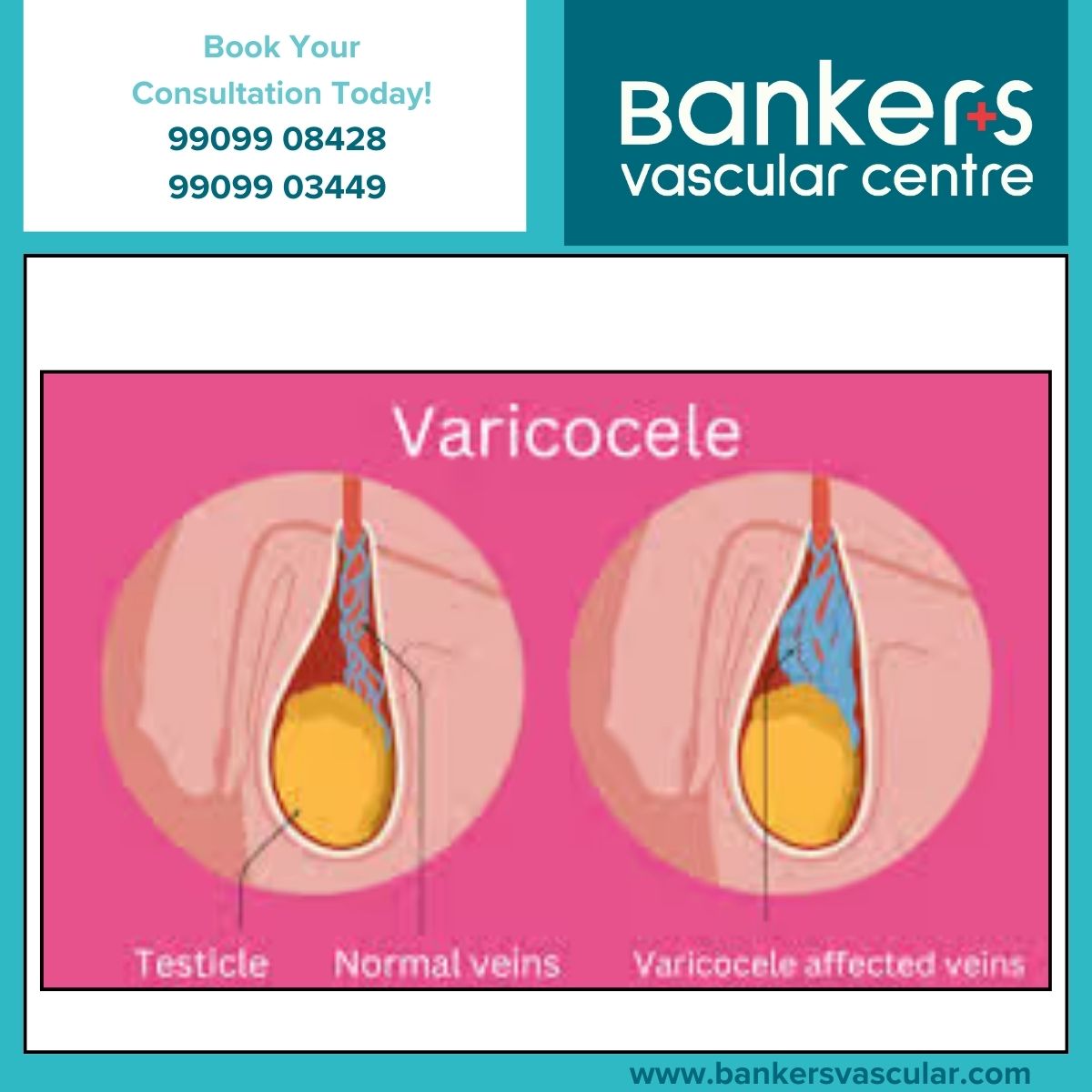
Varicocele
Instead of surgical vein ligation, varicocele embolisation treats enlarged veins using coils or agents delivered through a catheter. Patients typically walk out the same day.
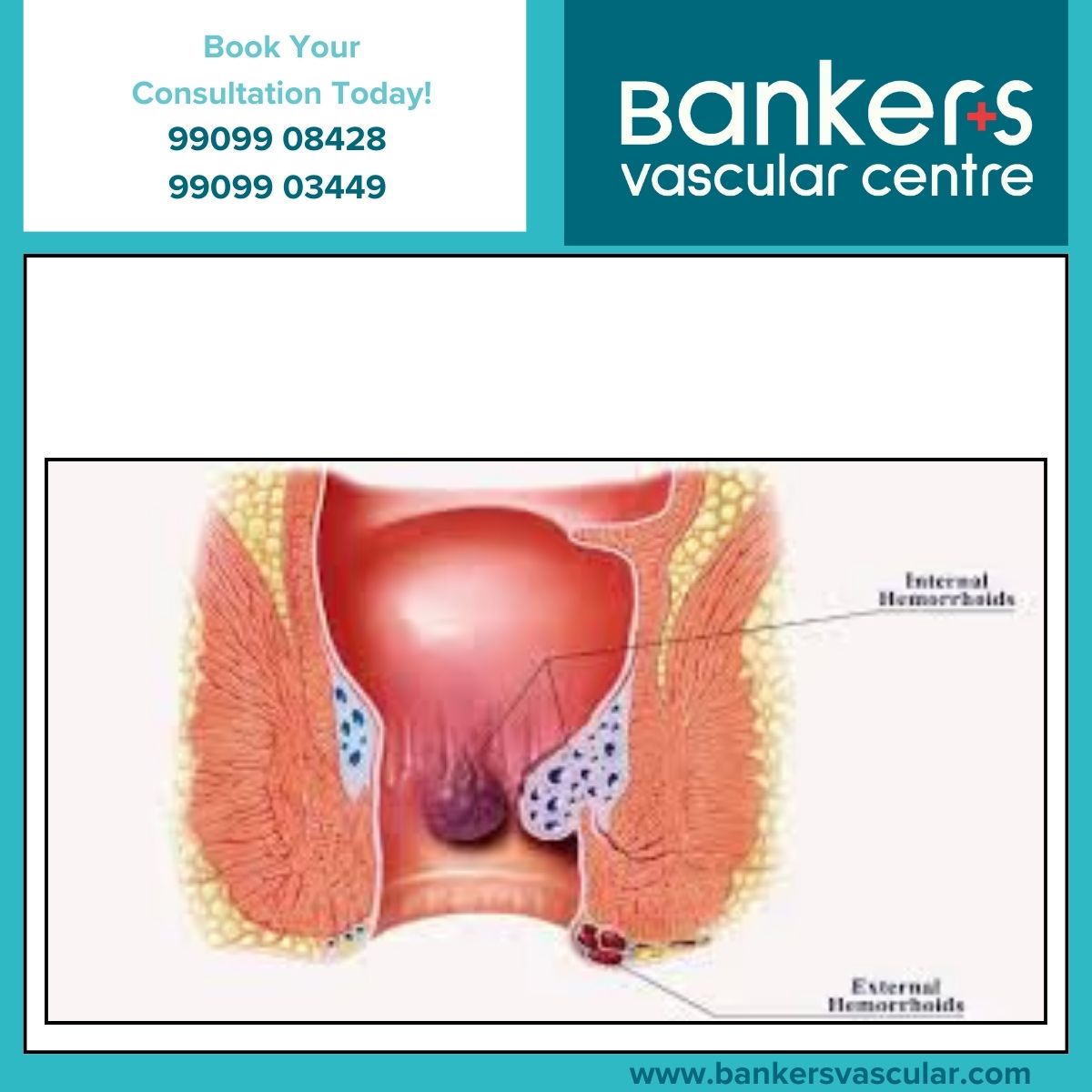
Hemorrhoids
Hemorrhoidal artery embolisation offers symptom relief without the pain and recovery associated with traditional hemorrhoid surgery.
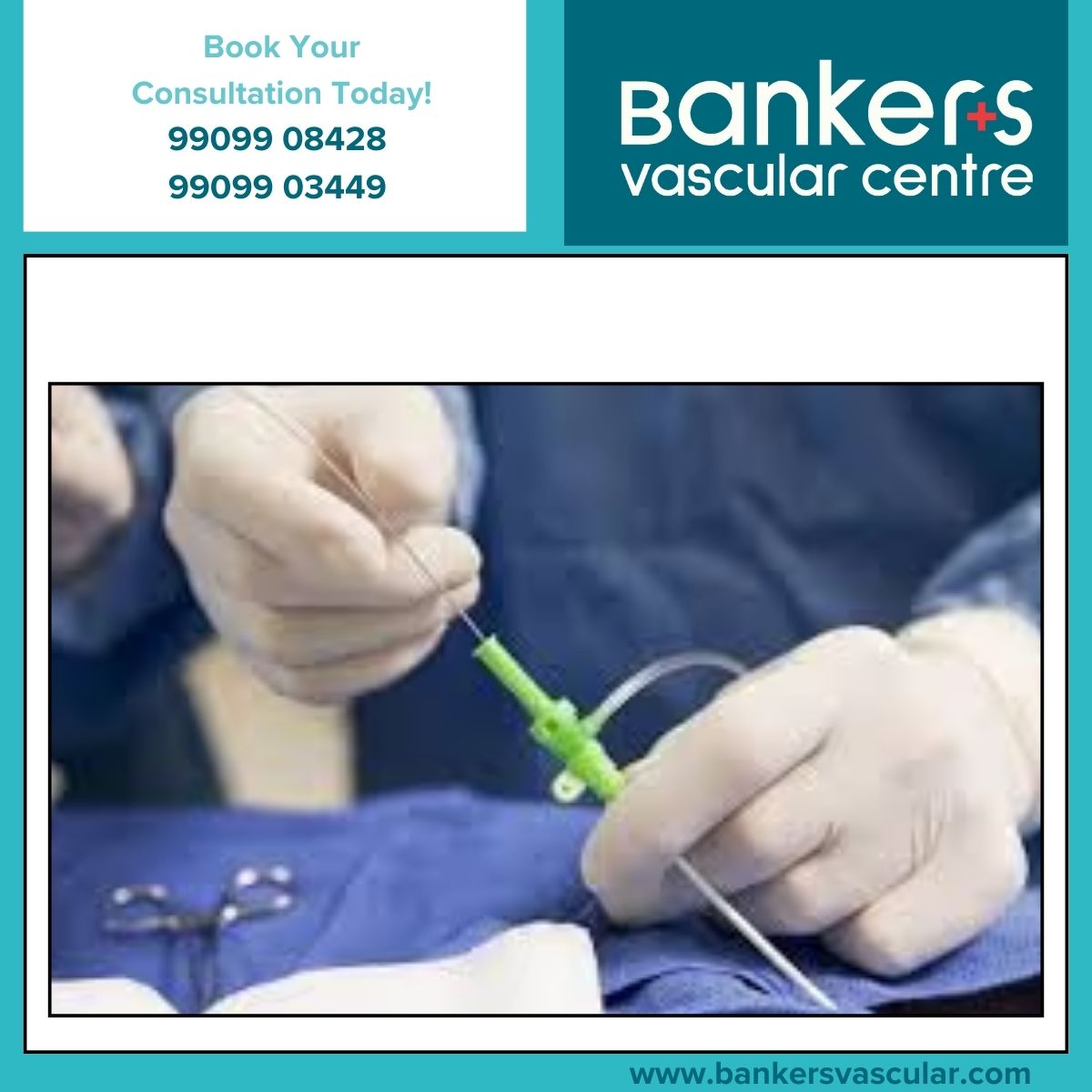
How the Procedure Works (Step by Step)
Local anesthesia and light sedation are given
A catheter is inserted through a small skin puncture
Imaging guides the catheter to the target blood vessels
Embolic materials are released to block blood flow
The catheter is removed and recovery begins
Are There Any Risks?
Like all medical procedures, embolisation isn’t risk-free. Possible complications include bruising, infection, allergic reactions to contrast dye, or incomplete treatment. However, for many patients, the risks are lower than open surgery.
Doctors carefully evaluate each case to determine if embolisation is the best option.
Why Embolisation was a 2025 Medical Breakthrough
Advances in imaging, catheter technology, and interventional radiology have turned embolisation into a frontline treatment — not just a backup option.
In 2025, it represents a shift in medicine toward:
For many conditions that once required surgery, embolisation is proving that smaller tools can deliver bigger results.

Comments
Post a Comment