Benign prostatic Hyperplasia
Introduction
- Prostate refers to a range of conditions that affect the prostate gland. a small, walnut-sized organ located just below the bladder in men. The prostate plays a crucial role in the male reproductivesystem by producing seminal fluid, which nourishes and transports sperm.
- Asmen age, the prostate is prone to several common health issues, which cansignificantly impact quality of life.
- Prostate pain is a comm but often misunderstood problem.
What does Prostate Pain feel like?
- Pain ordiscomfort in the lower pelvis or groin.
- Aching betweenthe scrotum and anus.
- Pain duringurination or ejaculation.
- May spread tolower back, thighs or genitals.
Prostate Pain
This may accompany either syndromeor both and is usually described as;
Causesof Benign prostate Hyperplasia
· Age
· Family History & genetic Predisposition
· Ethnicity
· Hormonal
· Obesity
· Sedentary Lifestyle
· High fat diet

Commoncauses of Prostate pain?
1. Prostatitis: Inflammation, often withinfection.
2. Benign Prostatic Hyperplasia: Enlargement ofthe prostate.
3. Prostate Cancer: May cause pain in advancestage.
4. Others: UTI, nerve pain, chronic pelvic painsyndrome.
Types
1. Irritative Syndrome
These aresymptoms caused by bladder irritation, often seen in conditions like prostatitisor benign prostatic hyperplasia.
Common Irritative Symptoms
2. Obstructive Syndrome
These symptomsresult from urinary outflow obstruction, usually due to prostate enlargement or inflammation, which blocks the normal flow of urine.
🔹 Common Obstructive Symptoms:
Investigation
1. USG + KUB + PVR
(Postovoidal Residual volume)
Complicationof BPH
- Recurre4ntunitary retention
- Chronickidney disease
- RecurrentUTI & bladder stone
- Hematuria
- Overflowincontinence
Management
1. Medication
2. SurgicalManagement
3. ProstateArtery embolization
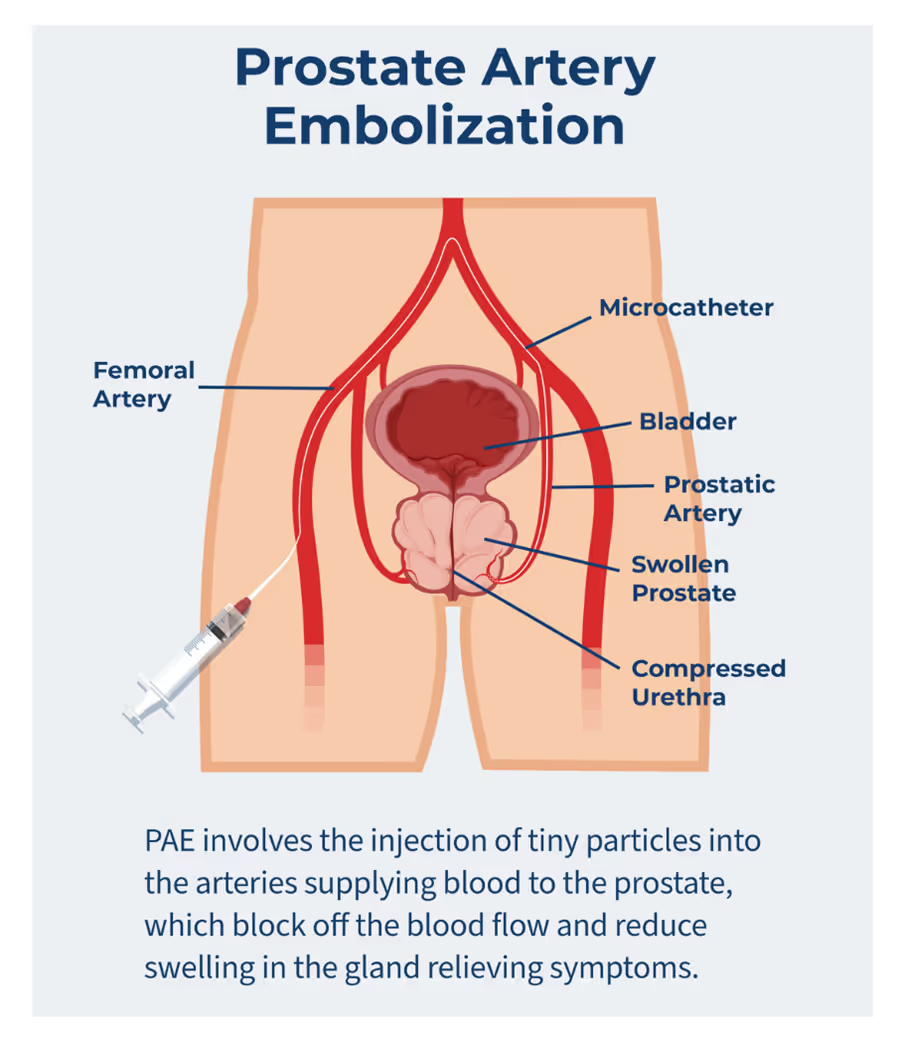
Procedureof PAE.
1. Pre-procedureevaluation:
o Imaging (like MRI, Doppler ultrasound) may bedone to map the prostate and its blood supply.
o Blood tests and urinary function tests may alsobe performed.
o Patient is typically given local anesthesia andsometimes conscious sedation.
2. Catheterinsertion:
o A small catheter is inserted into the femoralartery (in the groin) or radial artery (in thewrist).
o Using fluoroscopy (real-time X-ray), the interventional radiologist guides the catheter into the prostaticarteries, which supply blood to the prostate.
o Once the prostatic arteries are identified, tinyparticles (microspheres) are injected into them.
o These particles block the blood flowto the enlarged prostate tissue, causing it to shrink overtime.
4. Procedurecompletion:
o The catheter is removed and a bandage isapplied; no surgical incisions are made.
o The entire procedure typically takes 1.5to 2 hours.

Comments
Post a Comment